By clicking a retailer link you consent to third-party cookies that track your onward journey. This enables W? to receive an affiliate commission if you make a purchase, which supports our mission to be the UK's consumer champion.
What childhood rash is this?

It can be alarming if you discover a rash or spots on your baby or child, especially if you don't know what's causing it or what it could be.
Our guide includes photos of rashes on different skin colours, takes you through common causes of childhood skin conditions and explains what to do about them.
My child has a rash: what should I do?
Childhood rashes are common and usually harmless, and most will disappear without even needing treatment, but here's what to do if you spot one:
Rule out obvious causes. Have you recently changed your washing detergent or a baby product? Young skin is sensitive and more prone to irritation, inflammation and redness from something as basic as this. Switching to less allergenic formulations such as non bio detergent and treating with antihistamines in the meantime can help.
Is an infection going round? Check if they've been in contact with another child with a contagious illness at nursery, school or elsewhere, as this may give you a clue as to what the rash could be.
Do they also have a fever? Many rashes are accompanied by other symptoms such as fever – use a digital thermometer to check your child's temperature is within the safe range. Keep the thermometer in your first aid kit so it's always to hand.
If unsure, call 111 or contact your GP. If you're doubtful about what rash it is, get a professional opinion. For example, it can be harder to see rashes on brown or black skin, so the NHS advises you to check the soles of the feet, palms, lips, tongue and inside the eyelids for colour changes.
When to call 999 or visit A&E
In rare cases, a rash can be a symptom of something serious, such as an anaphylactic allergic reaction or meningitis. Call 999 or go to A&E now if your child has a rash and is unwell with any of these symptoms:
- A stiff neck
- Is bothered by light
- Seems confused
- A high temperature
- Has difficulty breathing (for example grunting noises or their tummy sucking under their ribs), breathlessness or fast breathing
- A rash that looks like small bruises or bleeding under the skin that doesn't fade when a glass is pressed against it
- Has skin that is pale, blue, grey or blotchy.
Meningitis rash
Meningitis is when the lining around the brain and spinal cord (the meninges) gets inflamed, usually because of a viral or bacterial (and, rarely, fungal) infection.
This can lead to meningococcal septicaemia (blood poisoning) with its telltale rash. It's a very serious illness that can cause widespread damage including skin and tissue damage, bone growth problems, organ failure and limb loss if not treated quickly.
Meningococcal septicaemia rash symptoms
- A reddish-purple, bruise-like 'petechial' rash caused by blood leaking into the tissues under the skin. Crucially, it doesn't disappear if you roll a glass over it.
- Fever, vomiting, cold hands and feet, rapid breathing, aversion to bright lights, a stiff neck, becoming floppy or unresponsive and an unusual cry or moaning.
Meningococcal septicaemia rash treatment
- Don’t wait for a rash – if you’re worried about any of these other symptoms, call 999 or go to A&E.
- The patient will usually be started on antibiotic treatment immediately and the treatment stopped if hospital tests show it's viral.
- Keep your child up to date with their vaccinations. Three doses of the MenB vaccine are given as part of the NHS vaccination schedule. Speak to your GP practice for further information.
Warning: 6 products that could pose a serious safety risk to your baby or child
Measles
Although it's less common than it used to be, measles is a highly infectious virus that's now on the rise in the UK because of fewer people getting the MMR (measles, mumps and rubella) jab.
Measles symptoms appear around 10 days after you’re infected, so it’s important to alert anyone your child may have been in contact with, including nursery and school.
Measles symptoms
- Cold-like symptoms including a high temperature, runny or blocked nose and sneezing.
- Grey-white spots on the back of the lips and inside of the cheeks, plus sore, red eyes.
- A red, blotchy measles rash a few days later (the rash doesn't tend to be itchy).
Measles treatment
- Plenty of rest, keep your child well hydrated and clean crusts from their eyes with cotton wool soaked in warm water.
- Give paracetamol or ibuprofen to relieve high temperatures.
7 things every parent needs to know about measles – symptoms to look out for, how to treat it and how to avoid catching it
Allergic reaction rash
Allergies in children are common – 40% of UK children have been diagnosed with one, according to Allergy UK – but they can still be a concern for parents.
Among the most common allergies in young children are food allergies (around 1 in 12), such as cow's milk allergy.
Allergic reaction rash symptoms
- Flushed face
- Hives on the face or a red, itchy rash around the mouth, tongue or eyes – possibly spreading across the body
- Blocked or runny nose
Allergic reaction rash treatment
- Hives can usually be treated at home by cooling the skin and administering antihistamines.
- If you detect swelling around their mouth or tongue or they have trouble breathing, ask for an urgent GP appointment or get help from NHS 111.
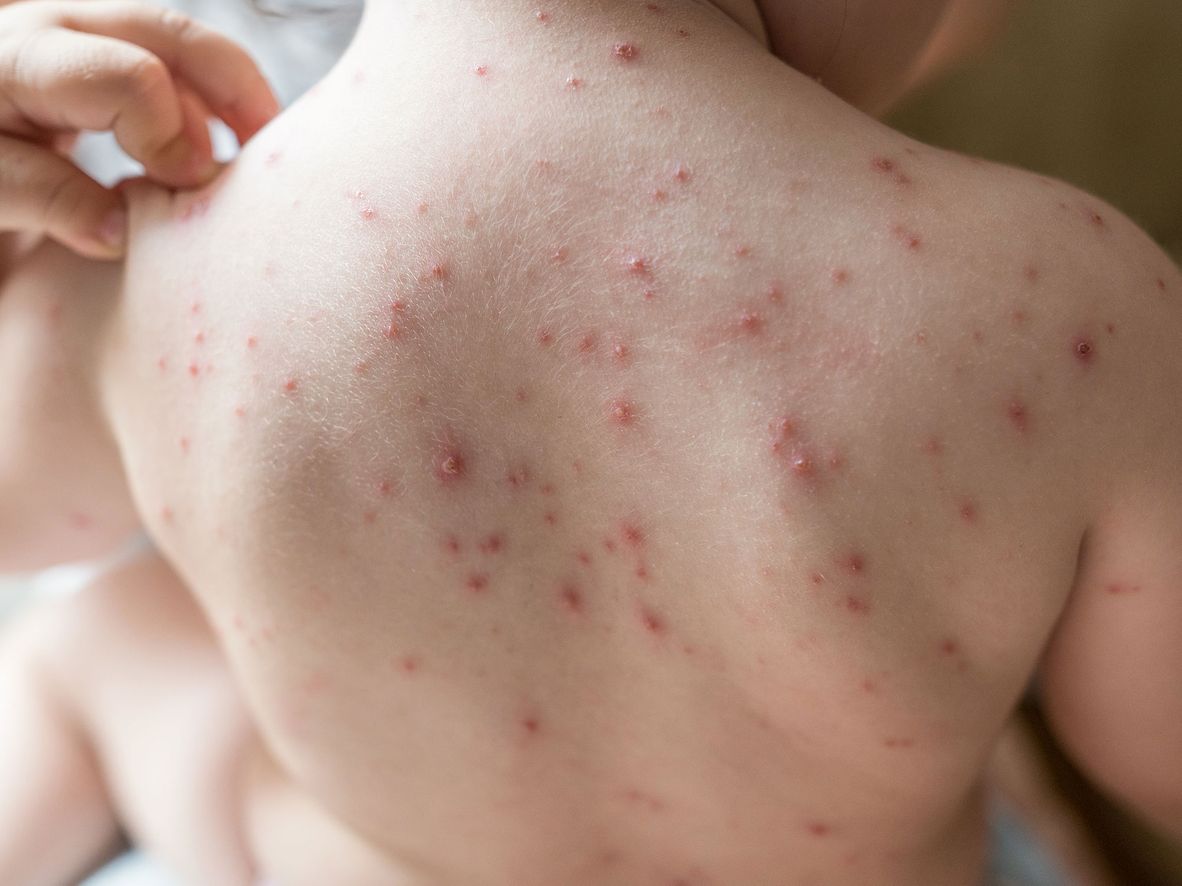
Chickenpox
Chickenpox is a common and very infectious virus that usually gets better by itself after a couple of weeks.
Chickenpox symptoms
- Stage 1: Small red spots appear. These can be anywhere on the body. Your child may also develop a fever, get aches and pains and lose their appetite.
- Stage 2: The spots become itchy, fluid-filled blisters.
- Stage 3: The blisters scab and may become flaky or leak fluid.
Chickenpox treatment
- Plenty of rest and hydration, plus antihistamines and paracetamol such as Calpol to ease itching. Avoid ibuprofen as it can cause skin reactions in people with chickenpox.
- Over-the-counter gels and foams for treating chickenpox scabs are easy to apply, less messy than calamine lotion and won't dry spots out.
9 things every parent needs to know about chickenpox – we give you the facts including what it is, how it spreads and how to treat it
Cradle cap
Although not technically a rash, the scales that are typical of cradle cap may still cause alarm if you spot them on your little one's scalp.
However, this common harmless condition – which is a form of seborrhoeic dermatitis – tends to go within six to 12 months, even if it's not treated.
Cradle cap symptoms
- Large patches of white or yellow scaly skin on the scalp, or the scalp can look pink with white or grey scales on black or brown skin.
- Mainly found on the head and face, but it can also appear in the nappy area.
Cradle cap treatment
- Lightly massage a moisturiser onto the scalp to help loosen the scales.
- Gently brush the scalp with a soft brush, then wash with baby shampoo. Don't be tempted to pick the crusts, as this can increase infection risk.
Best nit and head lice treatments – parents give their verdict on head lice treatments from brands including Boots, Full Marks, Lyclear, Nitty Gritty and Nitwits
Eczema
Eczema (atopic dermatitis) is a common skin condition that usually starts in babies and infants but tends to get better as they get older.
It can be worsened or even triggered by allergens such as certain foods, pollen or pets, products such as soaps and shampoos, or by factors such as central heating and hard water.
Eczema symptoms
- Itchy, bumpy, raised patches of skin that can appear anywhere but mostly on the hands, elbows, backs of the knee, face and scalp.
- Infected eczema oozes or weeps, has a scabbed yellow crust, is more itchy and painful than usual and the skin may be red or swollen.
Eczema treatment
- Emollients and wet wraps. Emollients are moisturisers used daily to prevent skin dryness, while wet wraps can help to cool the skin when symptoms worsen during an eczema flare-up.
- Steroids. Topical corticosteroids can be used intermittently to reduce skin redness and dampen inflammation during a flare-up. Calcineurin inhibitors may be prescribed if these don't work, especially for delicate areas such as around the eyes.
- Antihistamines and antibiotics. Antihistamines can help to relieve itching. Antibiotics can be prescribed if the eczema becomes infected (your GP may take a swab first).
Giant hogweed and other plant rashes
The milky sap from non-native giant hogweed (Heracleum mantegazzianum) contains high levels of photosensitising plant chemicals that make the skin unable to protect itself from UV light.
If you're in sunlight with the sap on your skin, it can cause a rash, followed by burning and blistering that can take around a week to heal. Even after this healing period, the skin can remain scarred and sensitive to light.
Giant hogweed symptoms
- Raised, red welts developing as quickly as 15 minutes after contact with the sap.
- Blistering if skin is exposed to sunlight/UV light.
Giant hogweed treatment
- Wash skin immediately with soap and cool water (don't burst any blisters), flush eyes with plenty of water as a precautionary measure and remove and wash clothing worn during contact.
- Get out of sunlight immediately (keep out for at least 48 hours) and seek medical advice. The Woodland Trust has information on giant hogweed and similar-looking but harmless plants such as cow parsley and common hogweed, plus other plants that can also cause phytotoxic burns such as wild parsnip or poison ivy (commonly found in the US).
Insect bites and stings: how to identify and treat them – what to look out for plus how to relieve the symptoms
Hand, foot and mouth disease
Hand, foot and mouth disease is a common childhood illness caused by a virus.
Despite the name, it has nothing to do with the foot and mouth disease that affects farm animals.
Hand, foot and mouth disease symptoms
- Sore throat, followed by mouth ulcers after a few days.
- High temperature and lack of appetite.
- Raised pink or red spots on the hands, feet and mouth (sometimes also on the thighs and bottom), turning into blisters that are grey or lighter than the surrounding skin.
Hand, foot and mouth disease treatment
- Antibiotics don't help hand, foot and mouth disease because it's viral, but the condition should get better by itself in 7 to 10 days (speak to your GP if it goes on for longer).
- Let them rest and give them plenty of fluids and soft foods such as yoghurt, but avoid acidic drinks such as orange juice and spicy foods as these can worsen mouth sores.
How can you cure tonsillitis quickly? Common symptoms, how long it lasts and the options for getting rid of it
Heat rash (prickly heat)
Heat rash is also known as prickly heat, sweat rash or miliaria. It occurs when sweat glands become blocked and, although it can be uncomfortable, it's largely harmless and can't be passed on to other people.
Babies get heat rash because they can't control their temperature as well as adults and children.
Heat rash symptoms
- Small, raised red spots with blisters that can look like beads of sweat.
- An itchy, prickly feeling.
- Redness and mild swelling.
Heat rash treatment
- Cool the skin by applying a damp cloth, giving them cooling baths or showers and dressing them in loose cotton clothing.
- Don't use creams or powders that can clog pores.
- Keep them well hydrated.
How to deal with heat rash and sunstroke – our guide to spotting the symptoms, plus check out our best baby and child sun creams
Hives (urticaria or nettle rash)
A hives rash, also known as urticaria or nettle rash, is usually caused by a reaction to food, medicines, pollen or insect bites and stings.
It's not to be confused with a nettle sting, which is caused by stinging nettle plants – the similar name is because the rash looks similar in both cases.
Hives symptoms
- Red, raised, itchy bumps or wheals, which can be in large patches or appear as red spots.
- Hives can be different shapes and sizes and can appear anywhere on the body.
- Itchy rash that can also feel like it's burning or stinging.
Hives treatment
- Damp compresses and cooling baths.
- Ask your pharmacist or GP for antihistamines that are suitable for children.
- If the hives keep coming back or don't improve after two days, visit your GP, as your child might have an allergy that needs to be investigated.
Hay fever symptoms and treatment options – we explain the options for symptom relief, plus how to save on medication
Impetigo
Impetigo is a highly contagious bacterial skin condition that's usually found on exposed areas such as the face and hands. It's particularly common in babies and young children.
Impetigo symptoms
- Reddish sores, often around the nose and mouth.
- These develop into fluid-filled blisters which, when burst, form a yellowish scab.
Impetigo treatment
- Hydrogen peroxide cream if it's in one area, or antibiotic cream or tablets if more widespread. Speak to your pharmacist, who can provide some of these treatments.
- Gently wash the scabs, cover them with loose clothing or bandages and stay away from others until they stop being contagious (48 hours after starting treatment or when patches are crusted over).
- Don't share flannels, towels or sheets with anyone with impetigo, and wash these at a high temperature after use.
How often should you wash your bedding? Follow these steps to keep your bed linen, pillows, duvet and mattress free from dust mites, dirt, sweat and dead skin cells
Nappy rash
Nappy rash is very common and is caused by moisture from urine and faeces irritating your baby's delicate skin.
Although mild nappy rash might not bother them too much, it can be uncomfortable, itchy and even painful.
Nappy rash symptoms
- Red, inflamed or spotty skin around your baby’s bottom and genitals.
- Skin may look shiny and sore and feel hot to the touch.
Nappy rash treatment
- Over-the-counter nappy creams will help to ease sore skin and act as a barrier to moisture to prevent it happening in the future.
- Change wet or dirty nappies as soon as possible and give your baby some nappy-free time each day to allow air to get to the skin. Place them on a waterproof mat in case of any accidents.
Best disposable nappies and nappy pants. Find out how parents rate Pampers and supermarket own-labels from the likes of Aldi, Asda, Lidl and Tesco
Ringworm
Despite the name, ringworm (also known as tinea) has nothing to do with worms: it's caused by a fungal infection.
Ringworm symptoms
- An itchy circular rash that's red or silvery in appearance and may also be scaly, dry or swollen.
- Ringworm can appear anywhere on the body, including the groin (known as jock itch) or the scalp (tinea capitis).
Ringworm treatment
- Use an over-the-counter antifungal product. Your pharmacist can advise, depending on your child's age and where the ringworm is, and can recommend if you need to see your GP.
- You may need to use the medication every day for up to four weeks. Stick to the instructions even if the rash has gone away.
- A child with ringworm can still go to nursery or school as long as they've started treatment, but let their teachers know they have it.
Roseola
Not to be confused with rubeola (which is what causes measles), roseola is a viral infection that causes a rash.
It’s most common in babies, toddlers and young children, although adults can also catch it.
Roseola symptoms
- Fever, sore throat, runny nose, diarrhoea, swollen glands and eyelids plus loss of appetite.
- Pinkish-red spots, bumps or patches, starting on the back and torso and spreading to the face, neck and arms.
- Some children may also have fits, known as febrile seizures, brought on by their high temperature.
Roseola treatment
- Plenty of rest and rehydration.
- If the fever makes your child uncomfortable, give infant paracetamol and get medical advice immediately if they have a febrile seizure.
Scabies
Scabies is caused by tiny parasitic mites that burrow into the skin to lay eggs, leaving lines with a dot at one end.
Although it's not usually a serious condition, it can affect anyone, including children and babies, and needs to be treated.
Scabies symptoms
- A bumpy, itchy, blister-like rash on the head, neck, palms and soles of the feet.
- Intense itching, especially during the night.
Scabies treatment
- A cream or lotion from your pharmacist to treat the entire family – this will need to be repeated a week later.
- Wash all bedding at 60°C and, if possible, put it in a hot dryer to remove traces of mites. Put clothing that can't be washed into a bag and seal it for three days until the mites die.
How to get rid of scabies in your home - our expert guide to getting rid of the highly infectious scabies bug from sofas, mattresses, towels, clothing and more
Scarlet fever
Scarlet fever (scarlatina) is a bacterial infection that mostly affects children.
Although in the past scarlet fever was a serious illness, antibiotics mean it's now less common and easier to treat.
Scarlet fever rash symptoms
- A bright-red rash that feels rough to the touch, like sandpaper.
- Your child may also get a temperature, swollen glands and a tongue that initially appears white before taking on a swollen ‘strawberry-like’ appearance.
Scarlet fever rash treatment
- Your GP can prescribe antibiotics, but call first rather than visiting the surgery because it's highly contagious.
- Scarlet fever is infectious for up to seven days before symptoms appear and until 24 hours after the first dose of antibiotic tablets are taken. Without antibiotics, you can spread the infection for two to three weeks after symptoms start.
- Relieve symptoms by drinking cool fluids, eating soft foods (if throat is sore) plus taking painkillers for high temperatures and antihistamines or calamine lotion for itching.
Best digital thermometers - our recommendations for those that will give quick and accurate results
Slapped cheek syndrome (Fifth disease)
Slapped cheek syndrome is cause by parvovirus B19. It gets its name from the bright-red rash on the cheeks that can look like the person infected has been slapped.
If you're pregnant and come into contact with anyone with slapped cheek syndrome, visit your GP or midwife immediately. The virus can be very dangerous for unborn babies.
Slapped cheek syndrome rash symptoms
- Feeling unwell for a few days, including high temperature, runny nose, sore throat and headache.
- A red cheek rash will appear a couple of days after this, followed by a raised, itchy, spotty rash across the body.
- Cheek redness and the body rash usually fade within two weeks.
Slapped cheek syndrome rash treatment
- As it’s a virus, there’s no medication for it.
- Relieve symptoms by drinking fluids to prevent dehydration and giving pain relief for high temperatures, headaches and joint pain.
- Use moisturiser on itchy skin and give antihistamines to relieve the itch.
Teething rash
Babies cut their teeth at around six months, on average. For some it passes without any symptoms, but for others it can cause issues.
Teething rash, sometimes known as a dribble rash or drool rash, is caused by babies dribbling as a new tooth pushes through and the saliva irritates their delicate skin.
Teething rash symptoms
- Red, inflamed skin on the cheeks, chin, neck and chest.
- Skin may be chapped, cracked or dry, including in the corners of their mouth.
Teething rash treatment
- Keep the skin on the face as dry as possible by dabbing away the drool.
- Ask your pharmacist for advice, as they may be able to recommend a topical cream to moisturise and protect the skin.
What to do if you're still unsure of the cause of your child's rash
You may still be uncertain about your child's rash or concerned about their symptoms, even after reading up on it and comparing the images.
You may also want clarification if the rash looks like it could be one of a number of things.
If this is the case, seek medical advice from your GP, pharmacist or by contacting NHS 111.