
Health? or Hype?
Make the right choice with recommendations you can trust, backed by expert testing.
Explore health recommendationsBy clicking a retailer link you consent to third-party cookies that track your onward journey. This enables W? to receive an affiliate commission if you make a purchase, which supports our mission to be the UK's consumer champion.

To find the best blood pressure monitors, we’ve taken more than 1,300 blood pressure readings. This means we can bring you our definitive verdict on the accuracy and ease of use of the most popular and widely available monitors.
Our accuracy tests involve assessing all blood pressure monitors against the AAMI/ISO Universal standard and the British & Irish Hypertension Society (BIHS) criteria.
Each monitor is tested on 15 participants, and all monitors are compared with mercury sphygmomanometer results, which is the current gold standard in blood pressure testing. Only the most accurate models passed both.
We focused on arm cuff blood pressure monitors in this test. Although wrist monitors tend to be lighter and more portable, they're more prone to giving inaccurate readings compared with arm blood pressure monitors, as your wrist isn't naturally at heart height.
How our tests find you the best
We've tested 10 blood pressure monitors
We've assessed arm cuff blood pressure monitors from big brands and at a range of prices to help you find one you can rely on.
Accuracy
Inaccurate readings are dangerous if you're relying on them to warn you about medical issues. Our robust tests separate the bad from the good.
Ease of use
You don't want an uncomfortable monitor that's a pain or overly complicated to use. Especially if you've got to take daily readings with it.
We also test...
How clear the instructions are, how easy it is to set up and how quick it is to use. Plus if there's any extra features or an accompanying app.
The biggest brands and the most popular blood pressure monitors are listed below.
Only logged-in Which? members can view the blood pressure test results.
Join Which? to get instant access to our test results and Best Buy recommendations.
| Blood pressure monitor | Price | Accuracy (AAMI/ISO Universal standard) | Accuracy (BIHS standard) | Ease of use | Features | Time taken (seconds) |
|---|---|---|---|---|---|---|
| Boots Advanced Blood Pressure Monitor | SQUIRREL_TEXT_50023639 | |||||
| Boots Multi-User Blood Pressure Monitor | SQUIRREL_TEXT_50023645 | |||||
| Braun ExactFit 3 | SQUIRREL_TEXT_50023656 | |||||
| Braun ExactFit 5 Connect | SQUIRREL_TEXT_50020252 | |||||
| Kinetik Wellbeing Blood Pressure Monitor | Argos (£18) | |||||
| Kinetik Wellbeing Fully Automatic Blood Pressure Monitor | SQUIRREL_TEXT_50023647 | |||||
| Omron Evolv | SQUIRREL_TEXT_50007146 | |||||
| Omron M2+ | Boots (£39.99) | |||||
| Omron M7 Intelli IT Afib | SQUIRREL_TEXT_50023655 | |||||
| Withings BPM CONNECT | SQUIRREL_TEXT_50009487 |
Dates tested: October 2025. Page last checked: December 2025. We're not able to show every retailer and cheaper prices may be available
All the blood pressure monitors we tested are listed in alphabetical order below.
Only logged-in Which? members can view the best blood pressure monitors from our tests.
Join Which? to get instant access to our test results and Best Buy recommendations.

Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for two users, stores 100 readings, irregular heartbeat detector, movement detection, average reading, smartphone-compatible, 22-42cm cuff size, battery-operated, carry case
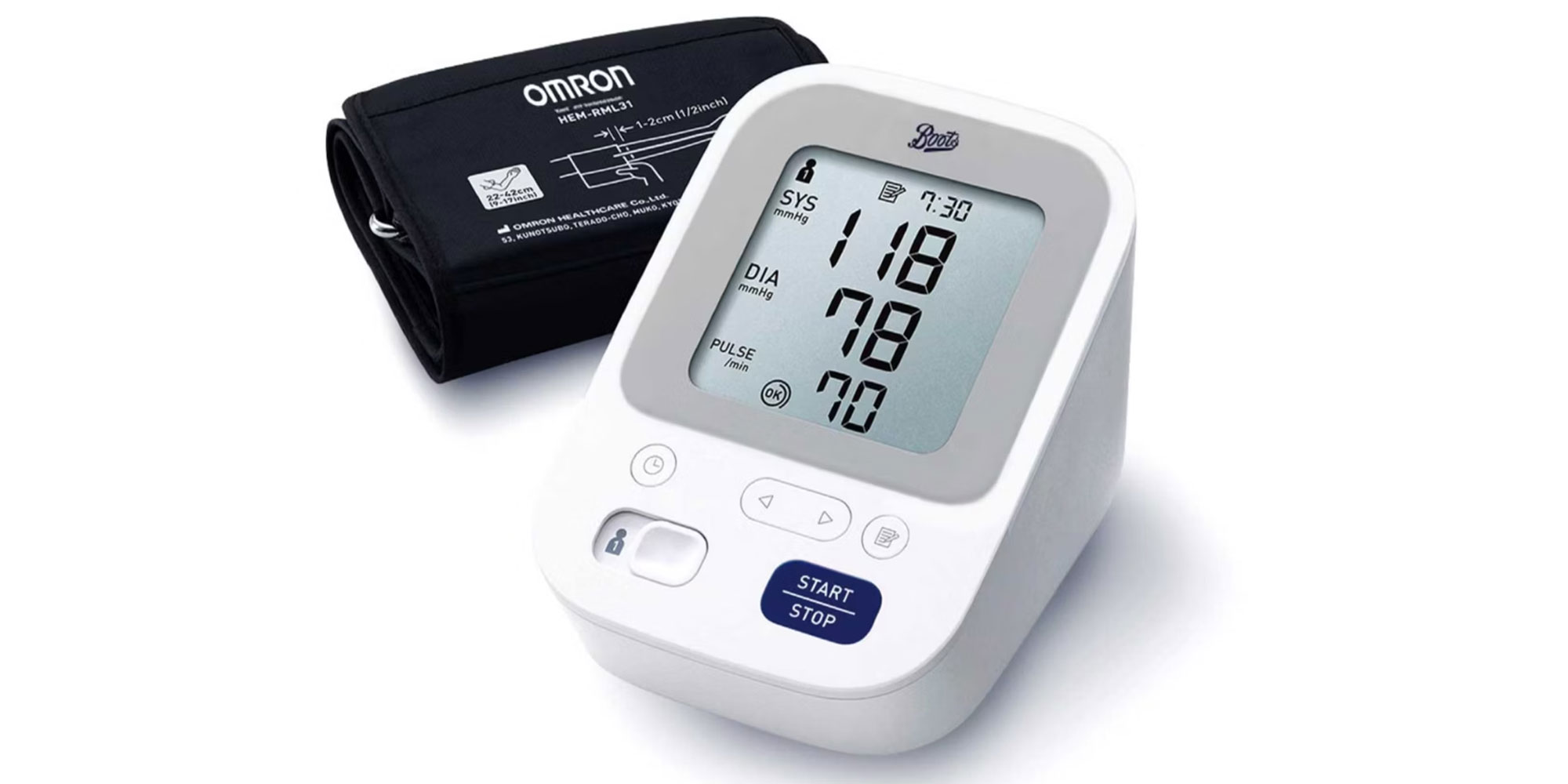
Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for two users, stores 60 readings, guest mode

Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for two users, stores 40 readings, irregular heartbeat detector, colour-coded hypertension indicator, 22-42cm/22-32cm/32-42cm cuff size, battery-operated, carry case

Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for two users, stores 60 readings, comparison function, irregular heartbeat detector, colour-coded hypertension indicator, smartphone-compatible, 22-42cm/22-32cm/32-42cm cuff size, battery-operated, carry case

Type Arm monitor
Need to know Saves readings for one user, stores 90 readings, 22-42cm cuff size
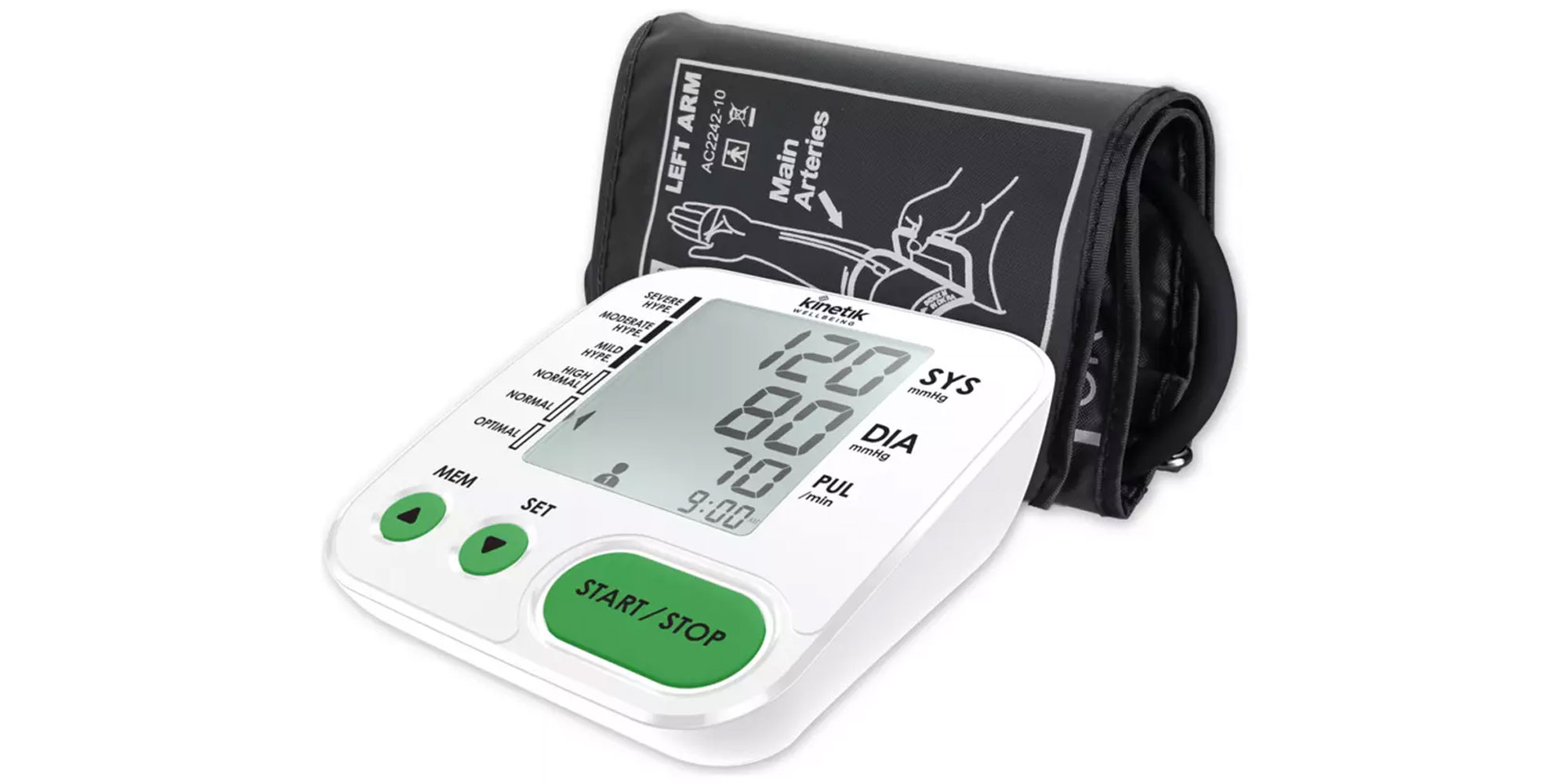
Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for one user, stores 90 readings, irregular heartbeat detector, 22-42cm cuff size, battery-operated, carry case

Type Arm monitor
Need to know Saves readings for two users, stores 100 readings, irregular heartbeat detector, movement detection, average reading, smartphone-compatible, 22-42cm cuff size, battery-operated, carry case

Available from Boots (£39.99)
Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for one user, stores 30 readings, irregular heartbeat detector, movement detection, hypertension indicator, 22-42cm cuff size, battery-operated, carry case

Most recently tested October 2025
Type Arm monitor
Need to know Saves readings for two users, stores 100 readings, guest mode, comparison function, irregular heartbeat detector, movement detection, hypertension indicator, smartphone-compatible, 22-42cm cuff size, battery-operated, carry case

Type Arm monitor
Need to know Saves storage for multiple users, stores 100 readings, guest mode, irregular heartbeat detector, movement detection, hypertension indicator, smartphone-compatible, data averaging, date and time stamp, 22-42cm cuff size, rechargeable, carry case
Our tests uncover the best and the worst. If a product performs so poorly that we think you should avoid it, we name it a Don't Buy.
We've tested two blood pressure monitors that are Don't Buys. These may be simple to use or have useful features, but if you can't rely on them to take accurate blood pressure readings, we can't recommend them. The Don't Buy products we found failed to meet the requirements of the British & Irish Hypertension Society (BIHS) criteria and the AAMI/ISO Universal standard. Meaning they failed to accurately measure either systolic or diastolic blood pressure.
To find out which they are, and which blood pressure monitors earned our Best Buy recommendation, log in or join Which?

Make the right choice with recommendations you can trust, backed by expert testing.
Explore health recommendations
We regularly revisit the blood pressure monitors on sale to see if any more popular brands need testing. If there are, we test them.
Find out more about how Which? is not influenced by product manufacturers or retailers and how your support helps us to stay editorially independent.

When we spoke with the Department of Health and Social Care, it confirmed that the NHS doesn't endorse medical devices.
Our investigation into non-compliant pulse oximeters sold on online marketplaces found uncertified models sold on Amazon, eBay and Wish, falsely claiming that these were endorsed by the NHS. Plenty didn't have the required CE marks to be sold in the UK, too.
Even if there are no definitive 'NHS-approved' blood pressure monitors, there are alternatives that come close. Seek out monitors displaying the British & Irish Hypertension Society (BIHS) logo and CE marking. You could also consult your healthcare provider for recommended blood pressure monitors.
Not any more. In late 2021, the NHS distributed free blood pressure monitors to 220,000 people diagnosed with uncontrolled high blood pressure as part of the Blood Pressure @home initiative.
However, in Somerset, every library is equipped with a couple of monitors available for borrowing. Pharmacies also offer free checks to eligible individuals over the age of 40. Visit this NHS eligibility tool to find a pharmacy near you if you qualify for free blood pressure checks.
Dr Pauline Swift, chair of Blood Pressure UK, answers your questions about blood pressure monitors

A healthy blood pressure reading is generally considered to be around 120/80 mmHg.
Anything consistently below 135/85 mmHg taken at home is usually considered acceptable in the UK, although elsewhere in the world, readings below 130/80 mmHg are considered appropriate; readings above 140/90 mmHg are typically classed as high blood pressure.
The ideal times are:
For a reliable picture of your blood pressure, it’s best to take two readings each time, a minute apart and repeat this over seven days. Your doctor will usually use the average.

The biggest mistake is not sitting in the right position. Things such as crossed legs, talking, dangling feet or having the cuff at the wrong height can all give inaccurate readings.
To get an accurate result:

The most important thing is accuracy. Look for devices that:
Additional useful features include:
Home monitors don’t need frequent servicing, but they should be checked for accuracy every one to two years. Some manufacturers offer calibration services.
Alternatively, you can take your monitor to your GP or pharmacy and compare it with their professional device. If a monitor has been dropped, damaged or gives erratic readings, it should be checked sooner